Merrillville, IN
Munster, IN
June 2024
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot or ankle to continually absorb the full impact of each step taken. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.
Stress fractures are common for individuals whose daily activities cause high levels of impact on their feet and ankles. Those who run, play tennis or basketball, or practice gymnastics tend to experience these fractures more frequently. Anyone is susceptible to this problem, though. Individuals who are normally sedentary and suddenly begin an intense, high impact workout may sustain stress fractures. This is because their muscles are not yet strong enough to handle and cushion the intensity of their activity. Osteoporosis may also cause someone to get stress fractures, because the disease weakens an afflicted person's bones and makes it easier for them to break down.
Pain from stress fractures typically occurs in the general area of the fracture. Pain can also manifest as “pinpoint pain” or pain that is felt when the site of the injury is touched, and can be accompanied by swelling. It may occur during or after activity, and it may disappear while resting and return when standing or moving. Engaging in any kind of activity, high impact or otherwise, will aggravate the pain. If the intensity of the activity increases before the stress fracture has properly healed, it can cause a full fracture.
Treatment can vary depending on the individual and the degree of injury. The primary way to treat a stress fracture is to rest the hurt foot. Some fractures will heal quickly with only a little bit of rest, while others may require a long rest period and the use of crutches, immobilization, or physical therapy. Under certain circumstances, surgery may be required to install support pins around the fracture to assist in healing.
If you are undergoing a new exercise regimen in running or some other kind of high impact activity, set incremental goals on a weekly basis so you can build up muscle strength. Make sure to wear supportive shoes to better protect you feet.
If you begin to experience any symptoms of stress fractures, you should stop exercising and rest. If the symptoms persist, consult with your podiatrist. Remembering these tips can help you prevent stress fractures to your foot and ankle, and allow you to continue living normally.
Causes and Risk Factors for Foot Stress Fractures
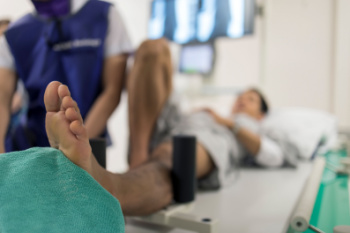
Stress fractures, common to runners and other athletes, result in placing excessive strain on the foot bones. One significant cause of stress fractures is a sudden increase in physical activity, whether it involves frequency, duration, or intensity. Transitioning from soft surfaces such as indoor tracks to harder ones like sidewalks can stress the bones of the feet. Improper technique due to foot conditions like blisters or bunions can also contribute by altering the foot's natural movement patterns and redistributing weight unevenly. Footwear that is poorly fitting, worn-out, or lacking proper support significantly increases the risk of stress fractures. While athletes commonly experience these injuries, non-athletes are also susceptible from extended walking on uneven terrain during vacations. Other risk factors for foot stress fractures, including osteoporosis, which reduces bone density and strength, as well as low vitamin D levels. Female athletes face other risks, possibly due to biomechanical differences, hormonal factors, and nutritional deficiencies. If you are experiencing pain in your foot after activity, it is suggested that you schedule an appointment with a podiatrist for appropriate testing and treatment options.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact Ahmad Elsamad, DPM from The Institute of Foot & Ankle Reconstructive Surgery . Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
- Gender – They are more commonly found in women compared to men.
- Foot Problems – People with unusual arches in their feet are more likely to develop stress fractures.
- Certain Sports – Dancers, gymnasts, tennis players, runners, and basketball players are more likely to develop stress fractures.
- Lack of Nutrients – A lack of vitamin D and calcium may weaken the bones and make you more prone to stress fractures
- Weak Bones – Osteoporosis can weaken the bones therefore resulting in stress fractures
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our offices located in Merrillville, and Munster, IN . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.
Tending to Bunions
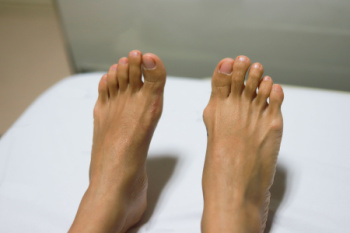 Bunions are bony bumps that form on the joint at the base of the big toe, causing the toe to deviate towards the other toes. They appear as swollen, protruding lumps on the side of the foot and can be red and tender. The condition can cause significant discomfort, including pain, swelling, and restricted movement of the big toe. Bunions often develop due to inherited foot structure, wearing tight or ill-fitting shoes, arthritis, or excessive stress on the feet. High heels and pointed shoes are common culprits in exacerbating bunions. Symptoms typically include pain, especially while walking, and inflammation surrounding the affected joint. Treatment for bunions ranges from conservative measures to surgery. Wearing wider shoes, using bunion pads, and taking anti-inflammatory medications can help to alleviate symptoms. Orthotic devices may help correct foot alignment. In severe cases, surgical intervention may be necessary to realign the bone and relieve pain. Untreated bunions can lead to complications such as bursitis or hammertoes. If you have a bunion that is causing you discomfort, it is suggested that you schedule an appointment with a podiatrist for treatment.
Bunions are bony bumps that form on the joint at the base of the big toe, causing the toe to deviate towards the other toes. They appear as swollen, protruding lumps on the side of the foot and can be red and tender. The condition can cause significant discomfort, including pain, swelling, and restricted movement of the big toe. Bunions often develop due to inherited foot structure, wearing tight or ill-fitting shoes, arthritis, or excessive stress on the feet. High heels and pointed shoes are common culprits in exacerbating bunions. Symptoms typically include pain, especially while walking, and inflammation surrounding the affected joint. Treatment for bunions ranges from conservative measures to surgery. Wearing wider shoes, using bunion pads, and taking anti-inflammatory medications can help to alleviate symptoms. Orthotic devices may help correct foot alignment. In severe cases, surgical intervention may be necessary to realign the bone and relieve pain. Untreated bunions can lead to complications such as bursitis or hammertoes. If you have a bunion that is causing you discomfort, it is suggested that you schedule an appointment with a podiatrist for treatment.
If you are suffering from bunions, contact Ahmad Elsamad, DPM of The Institute of Foot & Ankle Reconstructive Surgery . Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact our offices located in Merrillville, and Munster, IN . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Falls Prevention
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
How Seniors Can Prevent Falls in the Home

For seniors, falls can pose significant risks to health and independence, and can seriously impact the feet, necessitating the need to make fall prevention techniques in the home important. Start by ensuring adequate lighting throughout the house, especially in hallways, staircases, and bathrooms, to enhance visibility and reduce tripping hazards. Remove clutter and secure loose rugs or carpets to prevent slips and falls. Install grab bars in bathrooms and near toilets and showers to provide stability and support. Additionally, consider adding non-slip mats or adhesive strips to bathtub and shower floors. Keep commonly used items within easy reach to avoid overreaching or straining. Regular exercise to improve strength, balance, and flexibility can also reduce the risk of falls. Ensure that footwear fits well and provides proper support and traction. Regularly review medications with a healthcare provider to identify potential side effects that may increase fall risk. If falling has happened and foot conditions have arisen, it is suggested that you consult a podiatrist who can offer you effective treatment and additional prevention methods.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Ahmad Elsamad, DPM from The Institute of Foot & Ankle Reconstructive Surgery . Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our offices located in Merrillville, and Munster, IN . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Causes and Symptoms of Plantar Fasciitis

If you have ever felt a stabbing pain in your heel, especially when you first step out of bed in the morning, you might be experiencing plantar fasciitis. This condition, often referred to as painful heel syndrome or runner's heel, occurs when the plantar fascia, or tissue, that connects your heel bone to your toes becomes inflamed or tight. This causes intense discomfort, especially after periods of rest. Although plantar fasciitis is considered a repetitive stress injury, not just athletes are at risk. Anyone who spends a lot of time on their feet or has recently changed their exercise routine may develop plantar fasciitis. The pain is typically gradual, worsening throughout the day, and affects your ability to walk. It may even radiate toward your toes. While weight gain and sudden increases in activity can contribute to plantar fasciitis, it is essential to consult a podiatrist for proper diagnosis and treatment as other factors may be involved. A podiatrist is trained to assess this condition and recommend personalized treatment options, including stretching exercises, orthotic shoe inserts, or pain relief medication. Ignoring the symptoms of plantar fasciitis can lead to chronic heel pain or changes in your gait that may affect other parts of your body. For help in managing plantar fasciitis, it is suggested that you schedule an appointment with a podiatrist.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Ahmad Elsamad, DPM from The Institute of Foot & Ankle Reconstructive Surgery . Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our offices located in Merrillville, and Munster, IN . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.








